What Not to Say to Your Pain Management Doctor: Smart Communication Tips
Managing chronic pain can be a challenging journey. Pain management doctors are here to guide you, but the way you communicate can make a big difference. Saying the wrong things or not saying enough can affect your treatment plan.
Let’s dive into what not to say to your pain management doctor and how you can improve communication for better results.
Why Good Communication Is Essential in Pain Management
Your pain management doctor isn’t just guessing what might help, they rely on what you tell them. Clear and honest communication ensures they understand your symptoms and recommend the best treatments. However, some statements can send the wrong message or make their job harder.
Common Communication Mistakes
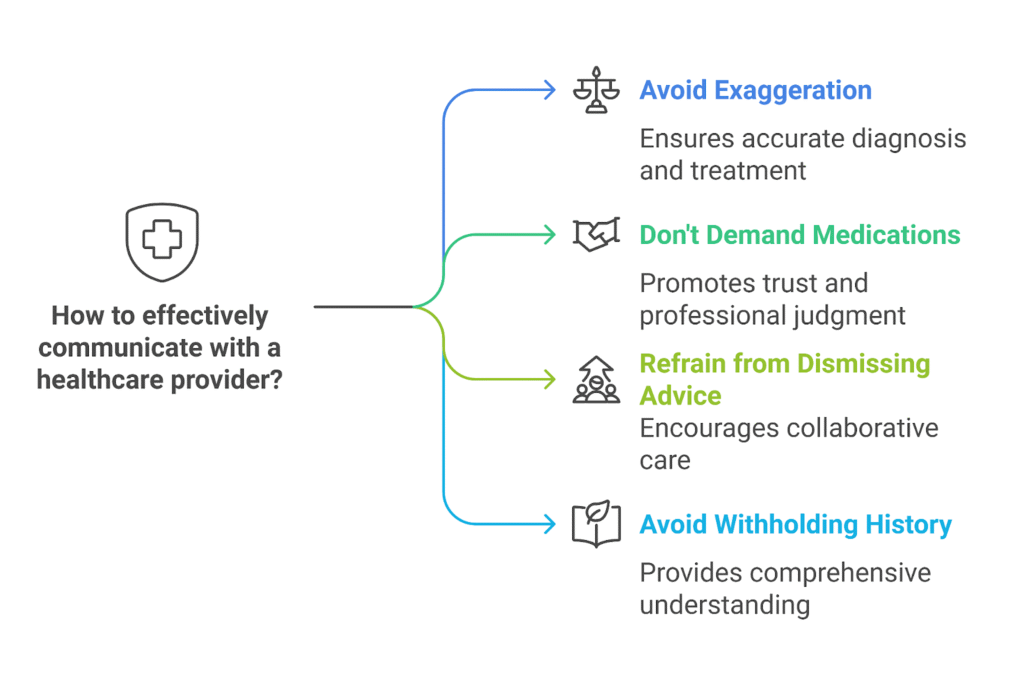
Before diving into specifics, here are some common missteps patients often make:
- Asking for a specific medication instead of discussing symptoms.
- Exaggerating or downplaying your pain.
- Avoiding questions because you’re embarrassed or unsure.
- Refusing treatment options without explaining why.
- Being dismissive of suggestions or plans.
Now, let’s look at specific things to avoid saying and why they might hinder your treatment.
What Not to Say to Your Pain Management Doctor
When talking to your pain management doctor, your words matter. Certain phrases can lead to misunderstandings or ineffective care. Here’s what not to say to ensure better communication and results.
1. “I just need [specific medi..tion].”
Asking directly for a treatment or prescribed treatment can raise concerns. Doctors might think you’re focused on medications or treatments rather than pain relief. Instead, describe your pain its location, intensity, and triggers. Let them suggest the most suitable treatments.
2. “Nothing ever works.”
It can feel like nothing helps when you’re in constant pain, but this statement doesn’t give useful information. Instead, explain what you’ve tried before and how it worked or didn’t. This gives your doctor a clearer picture of your history.
3. “My friend’s doctor gave them this medication.”
Every person’s pain is unique. Comparing your treatment to someone else’s might confuse the situation. Trust your doctor to consider your specific needs and medical history.
4. “I don’t have time for therapy or exercises.”
Your doctor might recommend physical therapy, lifestyle changes, or exercises to improve your condition. Refusing them outright could suggest you’re unwilling to take part in your recovery. If you have concerns, share them instead of dismissing their advice.
5. “I didn’t stick to the treatment plan.”
It’s okay if you struggled to follow a treatment plan. However, hiding this information can delay your recovery. Be honest about why you didn’t follow it, whether it was due to side effects, scheduling conflicts, or other reasons.
Real-Life Scenarios
Let’s break down specific situations where communication can go wrong and how to handle them.
When Asked About Pain Levels
- Don’t say: “It’s unbearable all the time.”
- Why: Doctors need details. Vague answers don’t help them understand how your pain changes.
- What to say instead: “My pain is sharp in the mornings, but it becomes dull after resting. It’s worse after walking long distances.”
When Discussing Doctor-prescribed Treatments
- Don’t say: “I’ve tried everything.”
- Why: It sounds dismissive and unhelpful.
- What to say instead: “I’ve tried over-the-counter medications like ibuprofen, but they didn’t work. Prescription treatment helped, but I had side effects.”
When Talking About Tests or Results
- Don’t say: “Why do I need this test? It’s a waste of time.”
- Why: Tests provide critical insights for your treatment.
- What to say instead: “I’m curious why this test is needed. Could you explain how it helps my treatment?”
How to Build Trust With Your Pain Management Doctor
Trust is a two-way street. When you communicate openly and show commitment, your doctor is more likely to create a plan that truly works for you.
1. Be Transparent
Tell your doctor everything about your pain, even if it feels small or embarrassing. For example, if your pain gets worse after eating certain foods or during specific activities, share that.
2. Keep a Pain Journal
Track your pain levels, triggers, and what helps. Writing it down can make it easier to explain your condition. A journal shows patterns that your doctor might use to adjust your treatment.
3. Be Open to Suggestions
Even if a treatment sounds unfamiliar or inconvenient, try to stay open-minded. Many options, like physical therapy, take time but can be effective.
4. Share Your Concerns
If you’re worried about side effects or the cost of a treatment, let your doctor know. They can often suggest alternatives or work with you to find a better solution.
The Role of Empathy in Pain-Management
It’s not just about what you say but how you say it. Your doctor wants to help you, so approach conversations with patience and empathy. Recognize that they are doing their best to find a solution that works for you.
Practical Tips for Better Communication
Here are some quick tips to improve your doctor visits:
- Prepare before the appointment: List your symptoms, questions, and concerns ahead of time.
- Be polite: Even if you’re frustrated, avoid being rude or dismissive.
- Focus on solutions: Discuss what’s working and what isn’t without negativity.
Communication Matters Everywhere
Clear words improve outcomes, whether in health or life. For ideas on inspiring messages, check out:
What to Say in a Retirement Card to Inspire Joy & Happiness – simple tips to write thoughtful, uplifting notes.
FAQs
Q. Can I ask for specific medications?
A. Yes, but it’s better to focus on describing your pain. Let your doctor determine the best medication for your condition.
Q. What if I don’t like a recommended treatment?
A. Be honest. Explain why it doesn’t work for you, and ask if there are other options available.
Q. How can I describe my pain better?
A. Use clear words like sharp, dull, throbbing, or burning. Share when it happens, how often, and what worsens or eases it.
Q. Why is honesty so important?
A. Honesty helps your doctor understand your pain fully. Without accurate information, they can’t design an effective treatment plan.
Final Thoughts
Your pain management doctor is there to help you, but they need your cooperation.
By avoiding what not to say to your pain management doctor and being open, you can work together for better results. Clear, honest conversations can lead to a plan that truly improves your quality of life.





